IMPLANT DENTISTRY
DENTAL CROWNS
DENTAL BRIDGES
Root Canal
SMILE AESTHETICS
Dental Veneers
IMPLANT DENTISTRY
DENTAL CROWNS
DENTAL BRIDGES
Root Canal
SMILE AESTHETICS
Dental Veneers

Myths about mouth ulcers are that they are a painful condition. While in most cases they’re harmless, they could take some time to heal.
Mouth ulcers are sore spots on the inside of the mouth that make chewing or brushing painful.
In this article, we will explore the nature of mouth ulcers, identify their common causes, and provide effective home remedies alongside pharmacy options. We’ll also discuss when it’s essential to seek medical attention.

They are small, open sores that form when a part of the soft lining inside your mouth or tongue breaks down. They most often appear on the inner cheeks, lips, tongue, or near the gums.
Ulcers are not contagious. They are distinct from cold sores, which typically occur around the mouth, are viral, and are contagious.
Ulcers take from two to three weeks to heal on their own.
Now, the common types you might see.
Ulcers take various forms because they can arise from multiple causes. Let’s explore the types of ulcers.

These are small, round ulcers that many people get repeatedly. They usually cause discomfort and tend to clear up within one to two weeks without special treatment. They may present as a single sore or multiple sores.

While this type of ulcer occurs naturally, some ulcers are caused by local injury.

Traumatic ulcers come from direct damage inside the mouth. Often, these ulcers are painful, but they heal immediately after the source of irritation is removed.
There are a range of reasons traumatic ulcers show, like biting your cheeks, a rough filing, or rubbing from braces. This type presents as a single sore. While traumatic ulcers exist due to individual habits or braces, Other ulcers point to infections or systemic issues.

Ulcers in this group are dangerous and must be tackled early. They are the result of a weakened immune system and are associated with disease.
Patients must immediately consult their GP or dentist to minimise the risk and pain of these ulcers.
These ulcers can happen for a wide range of reasons, such as;
| Related Illness | Cause | Accompanying Ulcers |
| Hand-foot-and-mouth disease | Viral infection (e.g., coxsackievirus) | Rash on the hands and feet, fever, sore throat |
| Oral thrush | Fungal infection (overgrowth of Candida yeast) | Creamy white patches on the tongue and inner cheeks, soreness. |
| Oral lichen planus | Chronic inflammatory condition | Lacy, white patches or red, swollen patches on the inner cheeks or tongue |
| Crohn’s-related ulcers | Inflammatory bowel disease | Abdominal pain, severe diarrhea, fatigue, weight loss, malnutrition |
Next, how these ulcers actually feel.
Ulcers are small, round or oval sores with a yellow or white centre and a red rim. They often cause discomfort during eating, drinking, or brushing. Areas surrounding these sores are either red or swollen.
Some patients report a tingling or burning sensation before the ulcer appears, which is your body’s way of talking to you. Typically, these sores are painful, but if they aren’t, it’s recommended to consult a physician early.
Patients who are under constant stress and are often fatigued can develop ulcers. These sore spots have multiple triggers, including certain foods, smoking, and certain fruits.
Patients should spot and avoid their personal triggers, as they can reduce the frequency of ulcers.
Ulcers are not caused solely by physical ailments; they can also result from lifestyle habits and physiological factors.
Sometimes ulcers can have underlying causes that are not apparent, such as the ailments mentioned above.
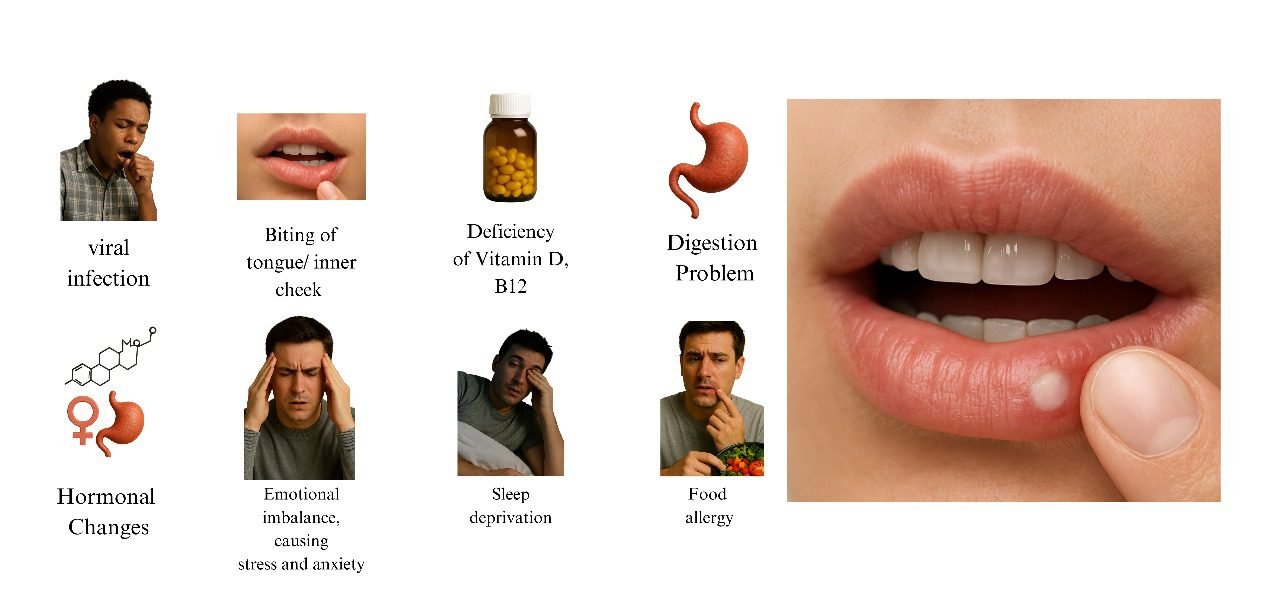
If a patient is suffering from severe or recurrent ulcers, it’s often linked to an underlying health issue such as;
If you frequently have mouth ulcers, it’s advisable to see a doctor or dentist. They can help you get tested to find out what’s causing them and recommend the best treatment.
On a positive note, most ulcers are treatable at home.
The majority of mouth ulcers will resolve without the need for prescription medication.
Some of the natural remedies include;
Now that we’ve explored the home remedies, it is time to discuss the clinical treatments.
Pharmacists can recommend a variety of over-the-counter products to manage the symptoms and promote the healing of mouth ulcers. These options help relieve pain and protect the ulcerated area.
Products such as topical anaesthetic gels and protective adhesive pastes are applied directly to the ulcer.
These help by creating a physical barrier that shields the sore from irritation while providing localised pain relief.
Certain mouthwashes contain antimicrobial agents like chlorhexidine.
These can help by reducing the bacterial load in the mouth and minimising the risk of secondary infection.
There are numerous myths surrounding ulcers and their treatment. Let us explore some of these myths and debunk the truth.
There have been some myths around ulcers, and we’re going to walk through them find the truth.
Common myths about mouth ulcers include:
Fact: Mouth ulcers, or canker sores, are not contagious. They are not caused by a virus and cannot be spread through kissing or sharing food and drinks. This is a key difference from cold sores, which are caused by the herpes simplex virus and are highly contagious.
Fact: Mouth ulcers (canker sores) and cold sores are different conditions. Mouth ulcers appear inside the mouth and are not contagious. Cold sores are blisters that typically form on the lips and are caused by a contagious virus.
Fact: While spicy or acidic foods can irritate an existing ulcer and make it feel more painful, they are not the direct cause of the ulcer’s formation.
Fact: The vast majority of mouth ulcers are benign and heal on their own within one to two weeks. However, if an ulcer is unusually large, persists for more than three weeks, or is accompanied by other symptoms such as fever or rash, it is important to seek medical advice to rule out an underlying cause.
While most mouth ulcers are benign and resolve spontaneously, it is advisable to seek medical evaluation if you experience any of the following:
A clinical assessment may involve diagnostic blood tests to check for nutritional deficiencies, management of any underlying conditions, or, in rare instances, a biopsy of a persistent ulcer to exclude more serious pathology.
Mouth ulcers are a common and typically benign oral condition that usually resolves within one to two weeks.
While basic at-home care is often sufficient for managing symptoms, specific products designed to ease discomfort and protect the ulcerated area are also available.
If an ulcer persists for more than two to three weeks, recurs frequently, or has an unusual appearance, it is important to seek a professional medical opinion.
Maintaining proper oral hygiene, balanced nutrition, and managing stress are key to long-term oral health. For product recommendations, such as those that provide a protective barrier and promote healing, consult a Doctor like Cem Baysal to get right to it.
